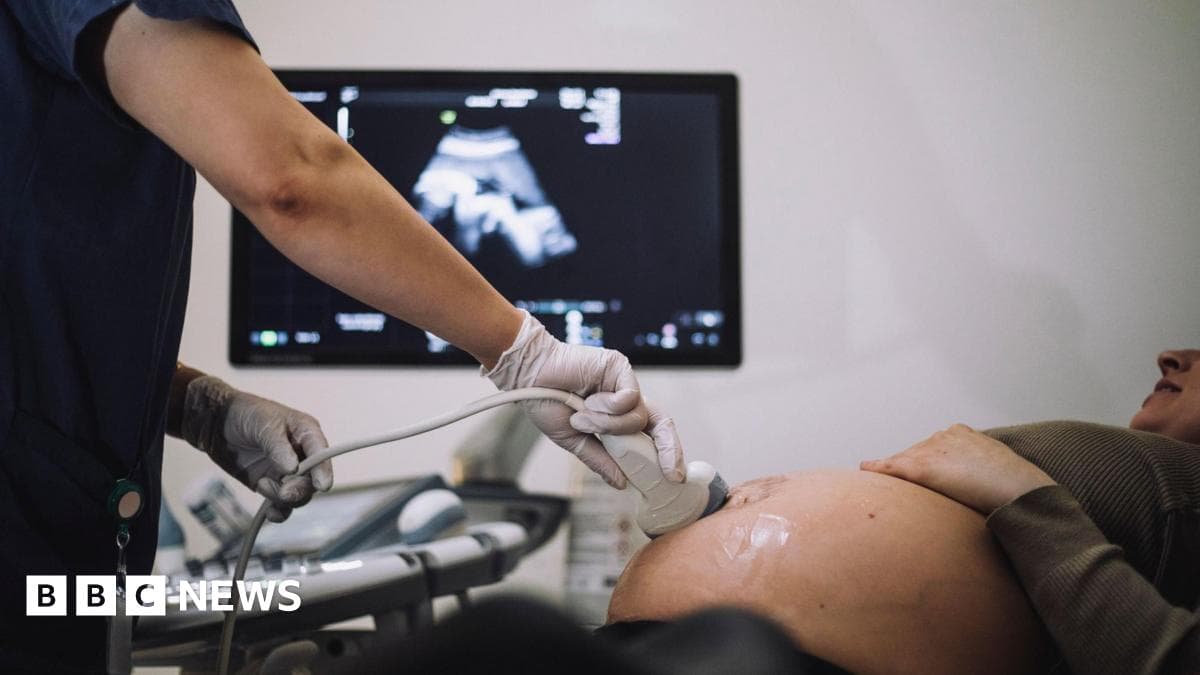
Better NHS care might have saved 58 babies, BBC finds
Key Takeaways
- Oxford University Hospitals Trust recorded 32 stillbirths and 26 neonatal deaths (2019-2024).
- BBC FOI findings suggest 58 babies might have survived with better care.
- Bereaved families cited missed chances and perceived arrogance in care.
Findings and scope
BBC findings show at least 58 babies at Oxford University Hospitals Trust (OUH) might have survived with better care between 2019 and 2024, including 32 stillbirths and 26 neonatal deaths, according to a Freedom of Information request.
“- Published At least 58 babies at an NHS maternity unit might have survived with better care, a BBC investigation has found”
The deaths involved babies referred to the trust for specialist care from across the region, and OUH said every baby death was reviewed in detail to understand what happened and whether improvements were required.

The investigation notes that between 2019 and 2024 OUH carried out 361 internal Perinatal Mortality Review Tools (PMRTs) into baby deaths, with at least 58 cases graded C or D indicating that different care may have been or was likely to have made a difference.
Contextually, separate BBC findings have pointed to hundreds of additional preventable baby deaths across the NHS in 2023 and 2024, including estimates of more than 800 nationwide, according to Sands and Tommy's Joint Policy Unit.
Personal cases and impact
Eleanor Taylor-Verlaan, 27, from Faringdon, Oxfordshire, says her daughter Alissa might be alive with better care.
Alissa suffered severe brain damage due to a lack of oxygen after the placenta came away from the womb wall, and Eleanor says she should have been seen straight away as she was high risk, with midwives' CTG monitoring overruled by doctors.

At 20 weeks a scan indicated higher risk of complications, but she was not closely monitored; at 35 weeks she complained of abdominal pains and sickness but was told to stay at home and take paracetamol.
On 20 February 2017, after waiting more than two hours in the maternity assessment unit, her baby was delivered by emergency C-section in poor condition; Alissa died six weeks later.
Eleanor says the care she received did not reflect her high risk status.
Separately, Alice Topping describes repeatedly trying to book an extra scan for her 40-week pregnancy, calling 44 times in one day; she says the trust prioritises scans at 36 weeks and her daughter Smokey died in September 2023.
An internal review found the trust did nothing wrong, but an independent investigation showed a catalogue of failings and made five safety recommendations which could have made a difference, which Alice believes should have been acted on.
Investigations and accountability issues
The BBC report notes that 27 baby deaths and 2 maternal deaths were independently investigated between 2019 and 2025 by the Maternity and Newborn Safety Investigations (MNSI), which identified key safety recommendations including foetal monitoring guidance, clinical assessments and oversight, risk assessments and better communication.
“- Published At least 58 babies at an NHS maternity unit might have survived with better care, a BBC investigation has found”
It adds that OUH paid out more than £72m in obstetrics compensation payments between 2020 and 2025, while Nottingham University Hospitals Trust paid about £61m.
OUH said its claims-per-birth rate was among the lowest compared with similar trusts that handle the most complex cases, and that compensation figures often relate to incidents from many years earlier and can be skewed by one or two high-value cases involving lifelong care needs.
Separately, the Care Quality Commission downgraded OUH's main maternity unit in 2021 to Requires Improvement, NHS England has placed targeted maternity support in place until June, and OUH is part of a national review of maternity and neonatal services due to conclude in June; the CQC issued a warning notice on 8 December 2025 for five breaches of regulation.
Oversight, accountability and responses
Campaign groups are pressing for accountability, with Families Failed by OUH calling for a judge-led public inquiry.
Health Secretary Wes Streeting has granted independent reviews into hospital trusts in Leeds and Sussex, but there are no plans for an Oxford inquiry yet.

Michelle Welsh MP, who chairs the All Party Parliamentary Group on Maternity, says there is a systematic toxic culture and that families deserve accountability and answers.
OUH's interim chief executive Simon Crowther told the BBC the stories were tragic and he recognised the lasting impact of losing a child, adding that the trust is willing to look at Eleanor's case again and reaffirmed its commitment to learning and improving the safety and quality of maternity care.
More on Technology and Science

Hawaii's Worst Flooding in 20 Years Threatens Dam, Prompts Evacuations as More Rain Looms
11 sources compared

Hawaii Deploys National Guard as Worst Flooding in 20 Years Swamps Oahu
68 sources compared

Heatwave shatters March records as Southwest bakes under extreme temperatures
48 sources compared

Record heat blankets the US Southwest as March logs hottest temperature in Arizona
10 sources compared